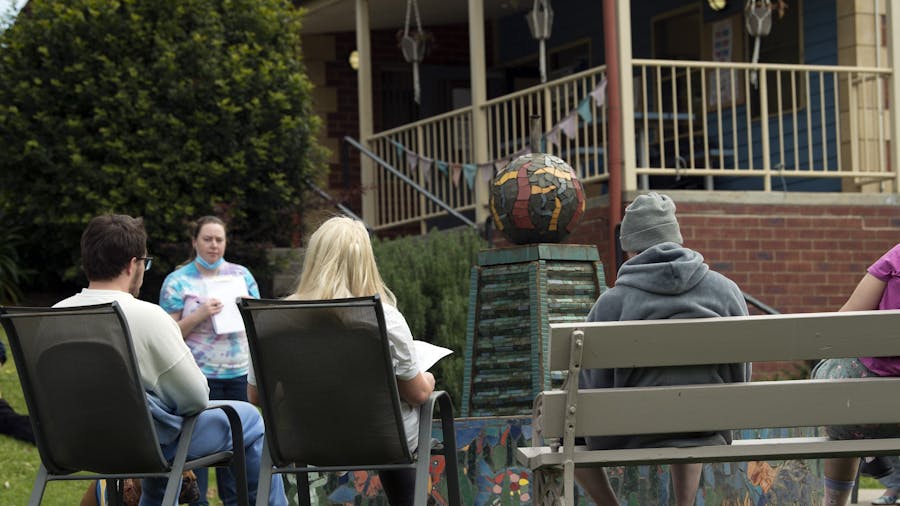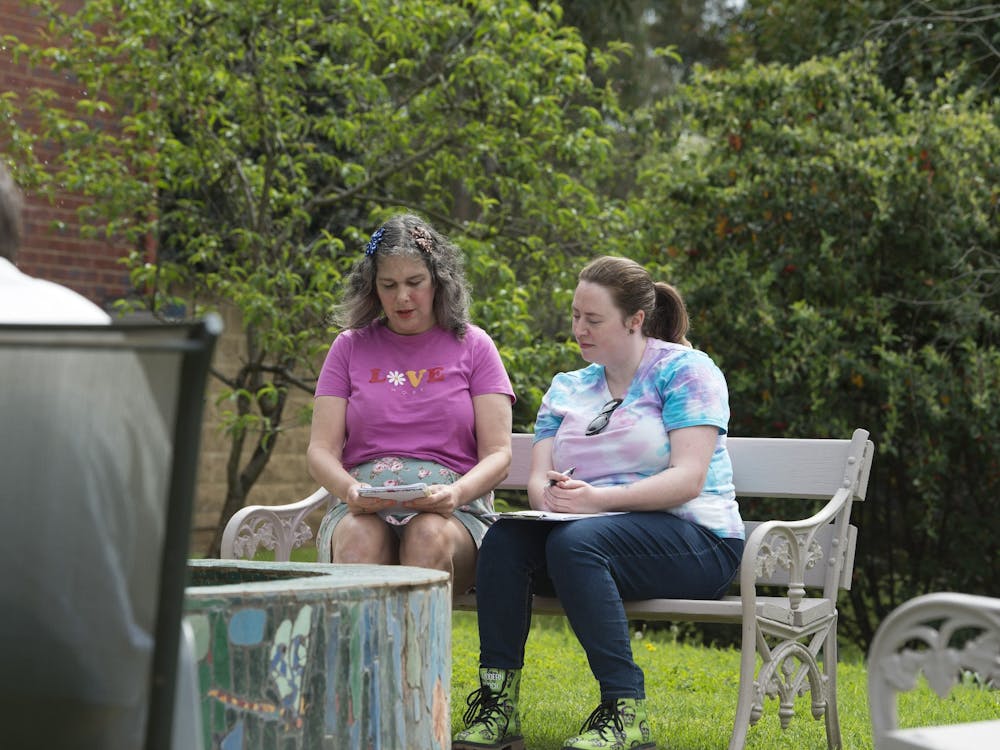Last year, our mental health triage service spoke to nearly 500,000 people from Melbourne's CBD, northern and western suburbs needing mental health support for themselves, their loved one or their patient.
Wellbeing and mental health support continues to be a major focus for the RMH. We are always there when it matters most.
Get help
Provide support
About us

Adult & older adult mental health services
We were the Royal Melbourne Hospital's Mental Health service. We focus on caring for adults and older adults in the inner city and western areas of Melbourne.

Child & youth mental health services
Orygen provides our youth mental health services. The Royal Children's Hospital cares for infants and children.
Sharing lived experience
Our recovery stories showcase the personal narratives and practical advice of people who live with a mental illness, or look after someone with a mental illness.
Latest news & events

The Royal Melbourne Hospital (RMH) has officially opened the Advanced Interventions in Mood Disorders (AIM) Clinic, marking a significant step forward in the treatment of severe mood disorders.

Today is R U OK Day, and today we’re addressing a very special elephant in the room.




A multi-instrumentalist and former consumer Arnaud LeBon has been using his talents to heal some of the RMH’s most vulnerable patients.
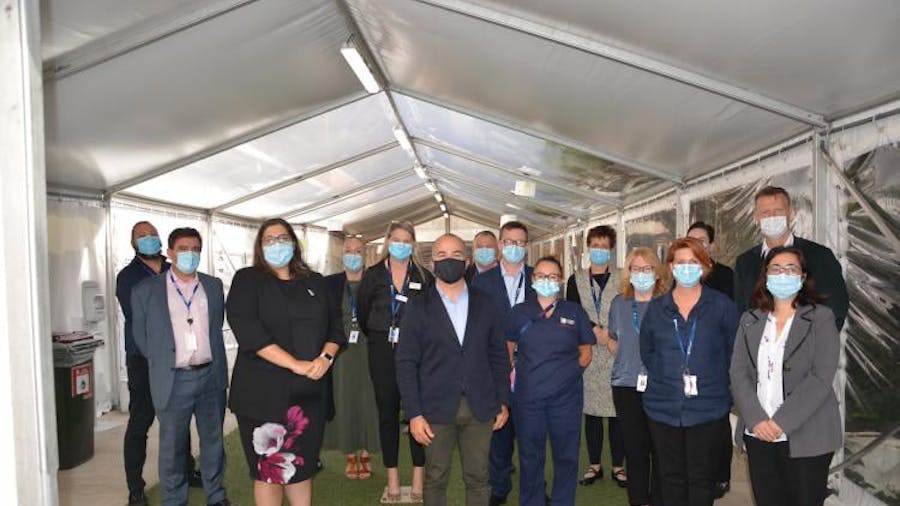
As one of the biggest providers of Mental Health services in Victoria, the Royal Melbourne Hospital’s NorthWestern Mental Health (NWMH) is excited to announce the launch of two new Hospital Outreach Post-suicidal Engagement (HOPE) services.